Bubble mattresses for bed sores, also known as alternating pressure mattresses, are critical medical devices designed to prevent and treat pressure ulcers – commonly called bed sores – in patients with limited mobility. These mattresses utilize an inflation and deflation cycle across different air cells, dynamically shifting the patient's weight distribution to relieve pressure on vulnerable areas like the sacrum, heels, and hips. The global incidence of pressure ulcers is significant, affecting millions annually and incurring substantial healthcare costs, making effective preventative measures like bubble mattresses essential. Understanding their function and benefits is paramount for healthcare providers and caregivers alike.
The demand for advanced wound care solutions, including bubble mattresses for bed sores, is rising globally due to aging populations, increasing prevalence of chronic diseases, and extended hospital stays. According to the World Health Organization, pressure ulcers impact an estimated 0.4% to 3.8% of hospitalized patients, with significantly higher rates in intensive care units. These injuries not only diminish quality of life but also contribute to prolonged hospitalization, increased infection risk, and elevated mortality.
Investing in effective pressure ulcer prevention strategies, such as utilizing a bubble mattress for bed sores, represents a proactive and cost-effective approach to healthcare. These devices not only mitigate patient suffering but also reduce the financial burden associated with treating advanced pressure ulcers, showcasing their importance in modern healthcare management.
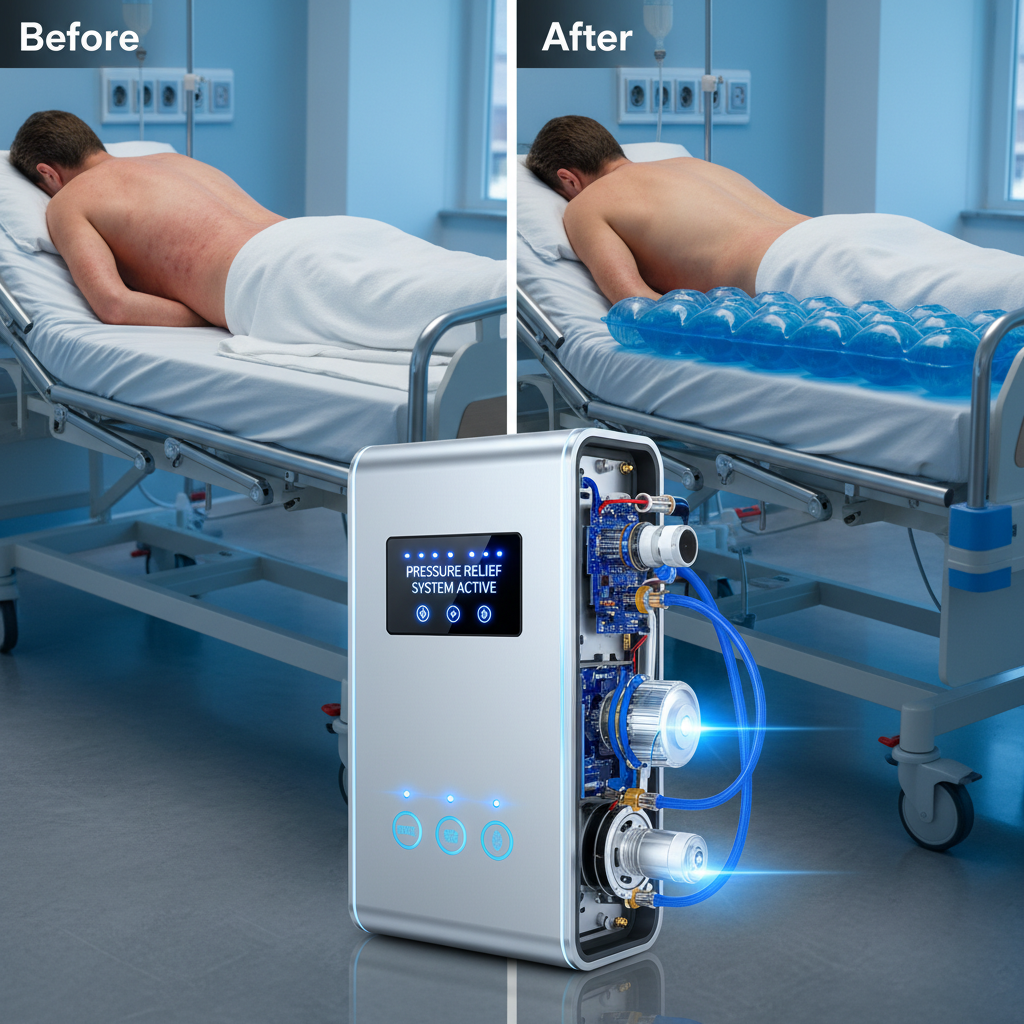

A bubble mattress for bed sores isn't simply an air-filled cushion; it's a sophisticated medical device engineered to actively combat pressure injuries. The core principle revolves around alternating pressure – a cyclic inflation and deflation of individual air cells within the mattress. This dynamic action prevents prolonged pressure on any single body part, encouraging consistent blood flow and minimizing tissue damage. The effectiveness of a bubble mattress hinges on factors like cell size, air flow rate, and the overall quality of construction.
These mattresses are crucial for patients confined to bed for extended periods, whether due to illness, injury, or surgical recovery. They are a cornerstone of preventative care, particularly in hospitals, nursing homes, and long-term care facilities, significantly reducing the risk of developing debilitating bed sores and improving patient comfort.
Bubble mattress technology utilizes a series of interconnected air cells that inflate and deflate in a sequential pattern. This cycling action creates a dynamic support surface that continuously redistributes a patient's weight, preventing sustained pressure on any particular area. The inflation pressure can often be adjusted to accommodate individual patient needs and weight ranges. Different models offer varying levels of air cell configuration and control features.
The simplicity of the core technology belies its effectiveness. The alternating pressure mechanism doesn't simply cushion the patient; it actively stimulates circulation, reducing the likelihood of tissue breakdown. This makes it distinct from static support surfaces like foam mattresses, which offer cushioning but lack the dynamic pressure relief of a bubble mattress.
Modern bubble mattresses are often constructed with durable, waterproof materials, making them easy to clean and maintain. Many also incorporate features like CPR valves for rapid deflation in emergency situations and quiet operation to minimize disruption to patient rest.
Durability is a paramount feature. A high-quality bubble mattress for bed sores should withstand continuous use and maintain its functionality over an extended period. This includes the robustness of the air cells, the integrity of the pump mechanism, and the resistance of the mattress cover to tearing and punctures.
Adjustability is equally critical. The ability to customize the inflation pressure to suit individual patient needs is essential for optimal pressure relief. Mattresses with multiple pressure settings allow caregivers to fine-tune the support provided based on a patient's weight, body type, and clinical condition.
Noise level is a frequently overlooked but important consideration. A quiet pump minimizes disruption to patient sleep and creates a more peaceful healthcare environment. Modern bubble mattresses often incorporate noise-reduction technologies to achieve near-silent operation.
Bubble mattresses for bed sores find extensive application in a wide range of clinical settings. Hospitals routinely employ them in intensive care units, surgical recovery wards, and long-term care departments to prevent pressure ulcers in immobile patients. Nursing homes and assisted living facilities utilize them proactively for residents at high risk of developing bed sores.
Home healthcare is another significant area of application. Patients recovering from surgery, suffering from chronic illnesses, or experiencing prolonged bed rest can benefit from a bubble mattress in the comfort of their own homes. Home health agencies often provide bubble mattresses as part of a comprehensive wound care plan.
The primary advantage of a bubble mattress for bed sores is its proactive prevention of pressure ulcers. By continuously redistributing weight and relieving pressure, it minimizes the risk of tissue damage and the formation of painful sores. This translates to improved patient comfort, reduced healthcare costs, and enhanced quality of life.
Beyond prevention, bubble mattresses can also aid in the healing of existing pressure ulcers. By offloading pressure from the affected area, they create an optimal environment for tissue repair and regeneration, accelerating the healing process and reducing the need for more invasive treatments.
The future of bubble mattress technology is poised for innovation, with ongoing research focused on enhancing pressure redistribution, improving patient comfort, and integrating smart technology. We are seeing the emergence of hybrid mattresses that combine bubble technology with other features, such as foam layers for added cushioning and temperature control.
Smart mattresses equipped with sensors that monitor pressure distribution and patient movement are also on the horizon. These intelligent systems can automatically adjust inflation levels to optimize pressure relief and provide real-time data to caregivers. Integration with telehealth platforms will further enhance remote monitoring and personalized care.
Sustainable materials and manufacturing processes are gaining traction, reflecting a growing commitment to environmental responsibility within the medical device industry. Expect to see more bubble mattresses constructed from recycled materials and designed for energy efficiency.
Despite their benefits, bubble mattresses are not without their challenges. Proper maintenance is crucial to ensure optimal performance. Regular inspection of air cells, pump functionality, and mattress cover integrity is essential. Failure to maintain the mattress can compromise its effectiveness and potentially lead to pressure ulcer development.
Skin care remains paramount even with the use of a bubble mattress. Patients should be regularly repositioned, and their skin should be kept clean and dry. Caregivers must be vigilant for any signs of skin breakdown and address them promptly.
Cost can be a factor, particularly for smaller healthcare facilities or individual patients. However, the long-term benefits of preventing pressure ulcers – including reduced healthcare costs and improved patient outcomes – often outweigh the initial investment.
| Maintenance Frequency | Skin Inspection Protocol | Patient Repositioning Schedule | Cost-Benefit Analysis |
|---|---|---|---|
| Daily visual inspection of air cells; Weekly pump function check | Every 2-4 hours; Document any redness or skin changes. | At least every 2 hours; Use a turning schedule. | Initial investment vs. potential cost of treating a pressure ulcer (estimated $5,000 - $15,000 per ulcer) |
| Annual pump replacement; Mattress cover replacement as needed. | Pay attention to bony prominences (sacrum, heels, hips). | Consider using a specialized turning device for patients with limited mobility. | Bubble mattresses can reduce hospital stays and associated costs. |
| Ensure proper pump airflow and filtration. | Early detection is crucial for effective intervention. | Document all repositioning efforts. | Long-term cost savings due to reduced incidence of pressure ulcers. |
| Follow manufacturer's guidelines for cleaning and disinfection. | Utilize a standardized skin assessment tool. | Adjust the schedule based on patient tolerance and clinical condition. | Reduced need for wound care supplies and specialized treatments. |
| Regularly check for air leaks and repair as necessary. | Report any concerns to the healthcare team. | Train staff on proper repositioning techniques. | Improved patient satisfaction and quality of life. |
| Proper storage when not in use. | Consider the patient’s risk factors for pressure ulcer development. | Involve the patient in the repositioning process whenever possible. | Minimizing the risk of litigation related to pressure ulcer development. |
Determining the ideal air pressure setting depends on the patient's weight and body type. Generally, a higher weight requires a higher pressure setting. Start with the manufacturer’s recommended setting and gradually adjust it until the patient is comfortably supported and there is no excessive sinking or bottoming out. Regular monitoring of skin integrity is vital.
Even with a bubble mattress for bed sores, regular repositioning is crucial. Patients should be repositioned at least every two hours to prevent pressure buildup in areas not fully relieved by the mattress. A turning schedule should be established and documented, taking into account the patient’s condition and tolerance. Consider using a turning device for patients with limited mobility.
Always refer to the manufacturer’s instructions for cleaning and disinfection. Typically, the mattress cover can be wiped down with a mild detergent and water. The pump should be regularly cleaned to prevent dust and debris buildup. Avoid using harsh chemicals or abrasive cleaners that could damage the mattress material.
Warning signs include unusual noises from the pump, inconsistent inflation and deflation of air cells, visible air leaks, or a noticeable decrease in pressure. If any of these issues arise, the mattress should be inspected immediately and repaired or replaced as needed. Continued use of a malfunctioning mattress can compromise patient safety.
Most bubble mattresses are designed to be compatible with standard hospital beds. However, it's essential to verify compatibility before use. Ensure the mattress fits securely on the bed frame and that the pump can be properly positioned and connected to a power source. Some beds may require specific adapters or modifications.
The lifespan of a bubble mattress depends on factors such as usage frequency, maintenance, and product quality. Generally, a well-maintained bubble mattress can last for 1-3 years. Regular inspection and timely replacement of worn-out parts, such as the pump, can extend its lifespan. Follow manufacturer’s recommendations for replacement.
Bubble mattresses for bed sores represent a vital component of comprehensive pressure ulcer prevention and management. Their dynamic pressure redistribution capabilities, combined with appropriate patient care practices, significantly reduce the risk of developing debilitating bed sores, enhancing patient comfort, and improving overall healthcare outcomes. Investing in high-quality bubble mattresses and prioritizing proper maintenance are crucial steps toward delivering optimal care.
Looking ahead, continued innovation in bubble mattress technology promises even more effective and patient-centered solutions. The integration of smart sensors, personalized pressure adjustments, and sustainable materials will further elevate the standard of care for patients at risk of pressure injuries. To learn more about our range of anti-bedsore mattresses and other patient care equipment, visit our website: bubble mattress for bed sores
If you are interested in our products, you can choose to leave your information here, and we will be in touch with you shortly.
